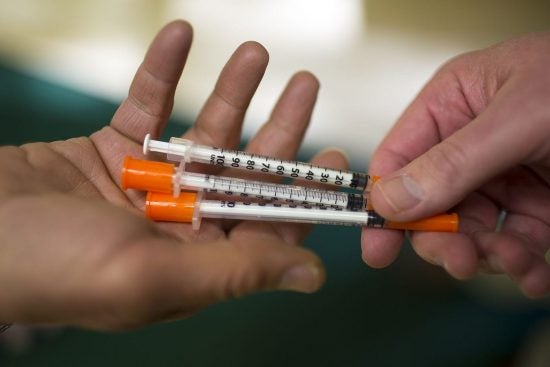
Injection drug use has been linked to outbreaks of HIV in several jurisdictions across the United States. In 2014-2015, Scott County, Indiana, experienced an outbreak that involved 181 people being diagnosed with HIV as a result of injection drug use. This HIV outbreak in a rural community that typically saw about 5 HIV diagnoses per year highlighted the vulnerability that exists in many parts of the country. In fact, the Centers for Disease Control and Prevention (CDC) has identified 220 US counties that have similar characteristics to Scott County and are most vulnerable to outbreaks of HIV and/or Hepatitis C.
In response to the Scott County outbreak and increasing urgency to address the opioid crisis, many jurisdictions took steps to establish syringe services programs (SSPs). SSPs are an evidence-based approach to reduce the transmission of HIV and Hepatitis C among people who inject drugs, and they offer a pathway to treatment and recovery from substance abuse. In 2015, then-Governor of Indiana Mike Pence signed into law a statute that allowed the establishment of SSPs by counties and municipalities in very specific circumstances, and in 2017, another law was passed that gave more authority to local governments to establish SSPs and extended the authorization period for these programs until 2021. Similarly, in 2015, the Kentucky legislature passed a law that allowed public health departments to establish SSPs after a process of receiving approval from relevant county boards of health, county fiscal courts, and city councils. In 2016, SSPs also became legal in North Carolina after the passage of a bill that allowed any governmental or nongovernmental organization that “promotes scientifically proven ways of mitigating health risks associated with drug use” to start an SSP.
Despite these legal authorizations and the expansion of SSPs in these states and in many other jurisdictions, problems with access remain. One reason is that there is a mismatch between the places where SSPs exist and places that have the greatest need for SSPs. A number of counties that are vulnerable to HIV and Hepatitis C outbreaks have no SSP. For example, West Virginia has 28 countries identified by CDC as most vulnerable for outbreaks, yet only nine of those counties have operating SSPs.
Even in counties that have SSPs, there are policies that create barriers to access. Cabell County has received attention for a recent HIV outbreak despite having an SSP. In Cabell County, the health department opened an SSP in 2015, but the county has reported a sharp rise in new HIV diagnoses among its residents. Since 2018, 80 people in the county have been diagnosed with HIV, and these diagnoses were primarily among people who inject drugs. Notably, Cabell County implemented a number of policy changes to its SSP starting in 2017, which have likely undermined the effectiveness of SSP services. Under these changes, first-time users of the SSP are only given 40 needles and the SSP expects to receive 40 back if the person wishes to continue with the program. The county also discontinued family members picking up syringes for individuals who use drugs, meaning that the individuals must come in themselves to pick up syringes. Additionally, and significantly, people who use the SSP must also be Cabell County residents and show proof of residency.
These kinds of policies exist or have been proposed in many other jurisdictions and are not effective in stopping the transmission of HIV through injection drug use. They are contrary to best practices that harm reduction advocates and health experts recommend. Best practices indicated that the following practices are counterproductive to effective SSPs: limiting the frequency of visits and number of syringes, enforcing a mandated exchange ratio (such as “one for one” exchange or providing new syringes only to those who return used ones), limiting program access to individuals who live within specified boundaries, requiring identifying documents, and requiring unnecessary data collection. These practices limit people who inject drugs from accessing SSPs.
The legalization and expansions of SSPs are critical to reducing the transmission of HIV and Hepatitis C and promoting health. But we also need to ensure that SSPs are not implementing policies that undermine this goal. More policy work is needed to eliminate barriers to people accessing SSPs. We must prioritize the needs of people who use drugs in health service delivery and ensure that people who use drugs have meaningful input into how SSPs operate.