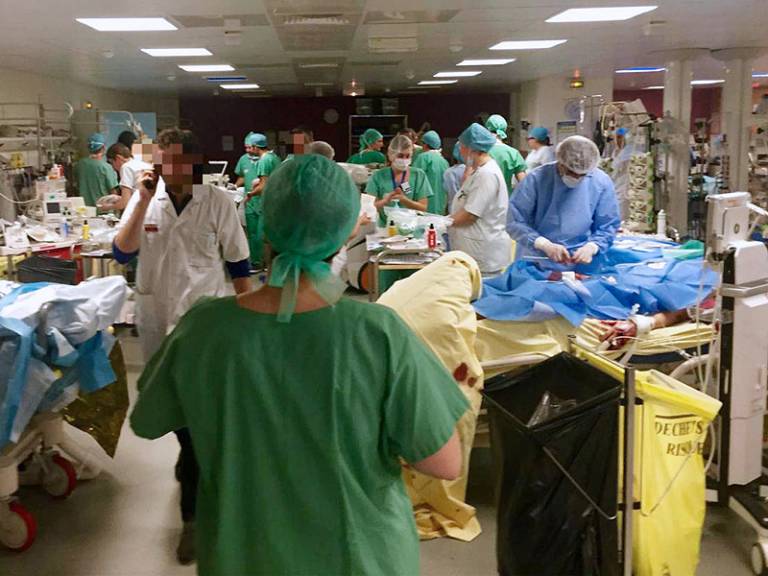
On November 13, Paris experienced the worst terrorist attack in the city’s history. In coordinated attacks across the city, terrorists detonated suicide vests and gunned down concertgoers. In the end 130 people were killed and more than 350 wounded—many seriously.
Mass casualty, multi-site terror attacks pose an extraordinary challenge to health system capacity. An influx of severely wounded people requires a coordinated response including a surge of medical personnel and first responders as well as complex coordination and triage. Most of all it requires careful preplanning.
Today, the Lancet released first-hand account of the medical response to the Paris attacks. Doctors who were directly involved in the aftermath detailed the mechanisms that were triggered by the attacks and how they worked in practice. As the authors note, “it is too early to report . . . the lessons that can be learned from this event.” Nonetheless, the article provides a fascinating look into how public health emergency preparedness.
The first thing that becomes clear from the article is that Paris had planned extensively for this sort of mass casualty event. The Assistance Publique-Hôpitaux de Paris (APHP) crisis unit can coordinate “40 hospitals . . . with a total of 100,000 health professionals, a capacity of 22,000 beds, and 200 operating rooms.” Once the scale of the attacks became apparent the APHP activated a crisis mode known as the White Plan. This included recalling staff to hospitals and releasing beds. This marked the first time the White Plan had been activated in the twenty years since it was developed.
Other hospitals in the area were used as “reservoirs” to provide surge capacity, and 10 helicopters were made available to transport patients. However, these were ultimately not needed as the main hospital alone was able to handle the influx. Service d’aide médicale d’urgence (SAMU), the Paris emergency medical services, were placed in charge of triage, while mobile units (a physician, nurse and driver) were sent to aid the wounded.
The report in the Lancet illustrates the response to a public health crisis in a city that was remarkably well-prepared. After the January 7, 2015 attacks on Charlie Hebdo, a satirical magazine in Paris that killed 11 and left 11 others injured, the city had been on high alert, rigorously planning and simulating the response to another attack.
In the end, of the patients who made it to the hospital there were “only four deaths (1%) among the 302 injured.” This included two patients who were dead on arrival. This remarkable success illustrates the power of vital role of public health preparedness. The Lancet article is an excellent read for anyone interested in the health system response to mass casualty events.
Latest
Breaking Cycles of Invisibility: Recent Advocacy Successes Putting Albinism Rights on the Global Health Agenda
Sarah L. Bosha Natalie Meyers Vilde Kvernstuen Grimsrud