Forty years ago, in June 1977, a nine-year old girl died of acute hemorrhagic fever at a hospital in Tandala, Zaire (now the Democratic Republic of Congo). Her post-mortem blood sample arrived at CDC-Atlanta nine days later, and despite the lack of refrigeration during shipping and its subsequent bacterial infection, scientists were able to positively identify the Ebola virus disease as the cause of death.
This new outbreak in Tandala – despite being defined as a single fatal case – and its subsequent investigation were significant in broadening our understanding of this new and horrible disease. This was the first naturally-occurring outbreak since Ebola was discovered and named nearly six months prior during the simultaneous outbreaks of Nzara, southern Sudan (now South Sudan) and Yambuku, northern Zaire, which killed more than 400 people, according to WHO. (NB: Another case of Ebola had since occurred by laboratory infection in England due to accidental stick of contaminated needle, but the single individual recovered.) To this day, scientists have been unable to determine any linkage between the Nzara and Yambuku outbreaks; in fact, they would not discover that they were separate outbreaks of two different strains for another four years, so in 1977, the virus was still “Ebola”.
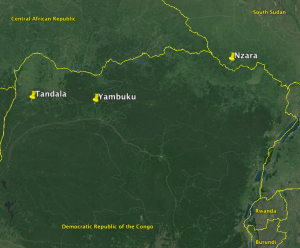
First, the Tandala outbreak extended Ebola’s endemic zone almost completely across the width of northern Zaire, along the Zaire (now Congo) River basin. The distance between Nzara and Yambuku is about 450 miles; the Tandala outbreak took place an additional 200 miles west of Yambuku in northwest Zaire. Tandala informed us that the previous outbreak was not just “a lightning strike”, and that the disease had a presence in the region.
Second, the epidemiological investigations that took place following the Tandala outbreak revealed that the virus had been circulating in the area, both before and after June 1977. One such investigation that took place from late 1977 to early 1978, found that two suspect cases at Tandala Hospital matched the case definition of Ebola, retrospectively, but no laboratory samples had been obtained from the two individuals, who had died in November and December 1977, six months after the June case. A family member of one of the deceased had been ill with similar symptoms and survived. Serum testing on the survivor revealed Ebola antibodies.
Additionally, investigators obtained serum specimens that had been drawn from missionaries in February 1977, four months prior to the June case. One of these individuals’ samples tested positive for Ebola antibodies. The individual, a Tandala Hospital physician, described being sick from Ebola-like symptoms in May 1972, five years prior to the June case, and almost four years prior to the Nzara-Yambuku outbreak. The physician, whose hospital records backed up his story, had lacerated his finger during the autopsy of another person who had died from a hemorrhagic illness that had been clinically diagnosed as yellow fever.
Finally, the investigation surveyed the area proximal to Tandala for historical or serological evidence of Ebola. After obtaining blood samples from 1,096 people from nearby villages, 79 individuals (7%) were found to have Ebola antibodies, despite no one being able to give an account of clinically severe Ebola disease.
After Tandala, there would not be another Ebola outbreak until July-October 1979, nearly two years later. That outbreak would take place, amazingly, in Nzara, the same Sudanese village from 1976… but, that is a story for another time.
40 years ago, Tandala showed us what we had been missing – the Ebola virus had been circulating for some time both before and after the 1976 outbreak, and in a wider area than previously known. Similarly, we are continuing to learn more in hindsight about other diseases that are affecting us today; a recent discovery has shown that Zika circulated freely and silently in West Africa for the last twenty years, and research is forthcoming that the virus circulated in Central Africa 35-45 years ago. These discoveries allow us to understand more fully the footprint of diseases, and stress the importance of looking backwards, as well as forwards, in order to best understand how to prepare for and detect disease outbreaks.
Tandala also showed us that the 1976 Ebola outbreak was not a “one-off”, and that we should be ready for it to emerge again. Today, we continue to emerge from the shadow of the 2014-2015 West African Ebola pandemic, the most catastrophic outbreak yet. Despite all we have learned about the virus in the last 40 years, there is still much we do not know, and are racing to discover, such as its natural reservoir, and how to vaccinate for and treat Ebola virus disease. Forty years and nearly thirty Ebola outbreaks later, we are still coming to terms with what we learned in Tandala in 1977.



