
Surveillance is an important part of tracking any disease because it serves as an early warning system, identifies public health emergencies, guides public health policy and strategies, and helps to understand and monitor the epidemiology of a condition to set priorities and guide public health policy and strategies. Zika is an excellent example of the importance of disease surveillance while highlighting some of the issues and concerns that arise, particularly when a disease moves from an epidemic into the post-epidemic period.
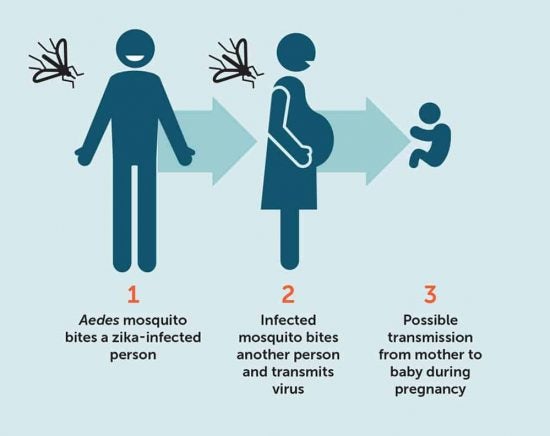
Zika virus disease is caused by a virus transmitted primarily by Aedes mosquitoes. Many people with Zika do not experience symptoms at all while others can have symptoms that are generally mild including fever, rash, joint pain, and headache that can last 2-7 days. Of concern, is the fact that Ziks virus is a cause of microcephaly and Guillain-Barré syndrome as well as other neurological complications when Zika is transmitted in utero, which can have long-lasting and devastating impacts on children and families. Links to other neurological complications are also being investigated.
While the exact time and place of the introduction of the Zika virus in the Americas is unknown, clusters of rash illness in Brazil’s northeastern states were being observed as early as November 2014. Following the increased detection of neurological anomalies including Guillain-Barré syndrome and congenital malformations of the central nervous system, the WHO Director- General declared that the cluster of microcephaly cases and other neurological disorders reported in association with Zika virus constituted a Public Health Emergency of International Concern (PHEIC) in February 2016, the fourth PHEIC ever declared.
Local transmission of Zika virus disease was reported in most countries in the Americas in the following months, leading to over 800,000 cases reported to the Pan American Health Organization (PAHO). Although Zika virus was first identified in 1947, we have learned more about the pathogen during the most recent outbreak than in the 70 years prior. However, there are still many questions regarding the full magnitude of the epidemic as well as specifications related to the impact of the central nervous system anomalies caused both by primary infection and through infection in utero.
WHO Surveillance Guidelines
According to the WHO Zika Surveillance Guidelines, “Zika surveillance should form part of each country’s national surveillance system and take into consideration any existing surveillance systems for other arboviral diseases, such as dengue and chikungunya, and diseases that may be part of the differential diagnosis, including, accid paralysis, measles, and rubella.”
WHO calls for integrated surveillance of arboviral diseases of public health importance including dengue, chikungunya, yellow fever, and Zika, which are all transmitted by the same mosquito vector. The integrated efforts should include epidemiological surveillance, laboratory surveillance, and entomological surveillance.
PAHO supports member states to implement integrated arbovirus surveillance. In September 2016 a regional strategy for Arboviral Disease Prevention and Control was approved by ministers of health from Latin America and the Caribbean at the 55th PAHO Directing Council. The strategy was developed to guide countries developing national action plans to strengthen surveillance, diagnosis, and case management. The strategy calls for:
- An integrated approach for arboviral disease surveillance, prevention, and control;
- Strengthening the capacity of health services of the differential diagnosis and clinical management of arboviral diseases;
- Evaluating and strengthening country capacity for surveillance and integrated vector control;
- Establishing and strengthening the technical capacity of the Arbovirus Diagnosis Laboratory Network of the Americas (RELDA).
Challenges and Concerns
A major concern is decreased reporting of Zika. Reporting is essential to surveillance. The international mandatory reporting requirement to WHO ended with the PHEIC in November 2016. Some countries have their own mandatory reporting requirements while others do not. Countries should be encouraged to continue reporting Zika cases to ministries of health and regional offices including PAHO.
The issue of privacy and protection is another concern related to data collection. Increased data brings increased challenges regarding protection and privacy. Regional data platforms that allow countries to upload disease data provide important information for disease surveillance but also raise privacy concerns. While these data platforms allow countries to upload their own data, and policies are in place to protect the data, there are concerns about the transferring of data and what happens when the data is sent from one source to another. This is an ongoing issue and organizations such as PAHO-WHO have protections in place to protect data.
One of the greatest challenges of Zika surveillance is that we have now transitioned into a post-epidemic period, meaning attention, resources, and funding have dwindled. This also impacts testing on the ground whereas less attention means clinicians are less likely to test for Zika when patients report symptoms that are similar to other arboviruses such as dengue and chikungunya. Integrating arbovirus clinical forms can help alleviate this problem by ensuring that all arboviruses are tested, including Zika even in a post-epidemic period.



