On March 26th, the Governor of Indiana, Mike Pence, declared a public health emergency in the rural southeast Scott County due to a severe outbreak of HIV. According to the Indiana State Department of Health (ISDH), out of the 4,200 people that live in this community, 142 have been diagnosed with HIV since December—this in a county that hadn’t recorded more than five cases in any prior year, with no reported cases in many of those years. 85 percent of those newly diagnosed HIV patients in Scott County are co-infected with the hepatitis C virus (HCV).
An investigation between the ISDH and the Centers for Disease Control and Prevention (CDC) linked the cause of the outbreak to the intravenous injection of oxymorphone, an oral painkiller sold under the brand name Opana. Abuse of the prescription opioid has been a common problem in southern Indiana for years and many other communities across the US. Scott County is one of the poorest and least healthy counties in Indiana and has struggled with injection drug abuse for years. Now the drug use in the area has spawned a second epidemic of a different kind: HIV and HCV.
Last Friday, CDC released a report showing that numbers are only set to rise. Among 112 persons interviewed thus far, 108 (96%) injected drugs; all reported dissolving and injecting tablets of the prescription-type opioid and using shared drug preparation and injection equipment. Those interviewed reported an average of nine syringe-sharing partners, sex partners, or other social contacts who might be at risk for HIV infection. The reported daily numbers of injections ranged from four to 15, with the reported number of injection partners ranging from one to six per injection event.
Sharing contaminated injecting equipment is one of the most efficient means of HIV transmission. The report emphasized the gravity of the problem—injection drug use in the community is multi-generational activity, with as many as three generations of a family and multiple community members injecting together.
Indiana’s initial response
The ISDH has developed a multipronged plan for dealing with the current outbreak. Among the measures are a public education campaign, a facility that offers immunizations, and programs that connect patients with addiction treatment centers and job training. While it is already concerning that these preventive measures weren’t in place to begin with, the most concerning is the controversial temporary needle exchange program that has been implemented. Gov. Pence—upon the recommendation of officials from the CDC—has temporarily suspended an Indiana law that bans needle exchange programs. Originally suspended for 30 days, the suspension has had to be extended due to the gravity of the outbreak for at least another 30 days. The needle exchange, which is limited to Scott County, started on April 4 of this year. As of Friday, 5,322 clean syringes had been provided to 86 participants, and about 1,400 used syringes had been returned. The center will also offer free HIV screening, drug treatment referrals and hepatitis A and B vaccinations. At this point, the people of Indiana should not be asking how long the law banning needle exchanges will be suspended for, but rather why it exists in the first place?
The irrefutable, yet controversial evidence in favor of syringe exchange programs
According to the CDC, the one-time use of sterile syringes remains the most effective way to limit HIV transmission associated with injection drug use. Needle exchange programs are the primary preventive measure for stopping HIV and HCV infections in communities of injection drug users. According to an overwhelming body of evidence, needle and syringe exchange programs not only reduce the spread of HIV and HCV, but also save money, encourage the safe disposal of syringes, minimize the risk of needlestick injuries to law enforcement officials, increase public safety and help drug users g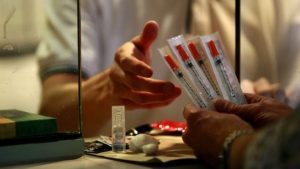 et into treatment, all without increasing drug use or resulting in other negative consequences. Yet, these programs are the most controversial, resulting in a number of legal and political barriers, both at the state and federal level. Currently, 25 states require a prescription to buy syringes while others have strict paraphernalia laws in place. Many states criminalize needle possession, arresting people as they leave private needle exchange facilities. Additionally, there is a federal ban in place banning any federal funding going towards syringe exchange programs.
et into treatment, all without increasing drug use or resulting in other negative consequences. Yet, these programs are the most controversial, resulting in a number of legal and political barriers, both at the state and federal level. Currently, 25 states require a prescription to buy syringes while others have strict paraphernalia laws in place. Many states criminalize needle possession, arresting people as they leave private needle exchange facilities. Additionally, there is a federal ban in place banning any federal funding going towards syringe exchange programs.
HIV remains one of the country’s most serious health challenges and CDC data shows that injection drug use accounts for an estimated 8% of the approximate 50,000 annual new HIV infections in the US. Additionally, contaminated drug-injecting equipment is the most frequent mode of transmission for HCV. Nationally, acute HCV infections have increased 150% from 2010 to 2013. Even with these numbers, only 28 states have removed or limited barriers to syringe distribution in prescription and paraphernalia laws while only 16 states and the District of Columbia explicitly authorize syringe exchange. Kentucky was the last state to do so on March 25th, precisely due to the concern of a growing HIV and HCV epidemic in their state.
The illegality of syringe exchange programs remains one of the biggest mysteries in the public health sphere. There are very few issues where the entire medical and health community can reach unanimous consensus. The World Health Organization, the CDC, the Substance Abuse and Mental Health Services Administration, the National Institutes of Health, the Institute of Medicine, the American Medical Association and basically every expert health group that has analyzed the data favors syringe exchange and legal needle access. More than three decades of overwhelming data now shows that needle exchange programs do tremendous good, while causing no discernible harm; the data on their safety and efficacy is stronger than for virtually any other public health intervention. The only reason to oppose them today is ignorance — or petty politics.
Last week, Governor Pence stated that he opposes clean needle exchanges as a drug addiction-fighting strategy, but is making an exception in the case of Scott County. “I don’t believe that effective anti-drug policy involves handing out paraphernalia to drug users by government officials,” he says. Not only does his stance on drug policy show a complete disregard for the facts; it also poses a danger to the Indiana population
. Earlier this month, The Indianapolis Star wrote that the addiction problem extended to neighboring Clark, Jackson and Washington counties, as well as nearby Perry — all near the Kentucky border. CDC has also warned that the US epidemic of opioid abuse could lead to more severe outbreaks of HIV and HCV nationally, much like the outbreak now seen in Indiana. This fear has lead some people in the state to call out for needle exchange legalization throughout the state. Rep. Ed Clere, a Republican state legislator who represents a nearby county, says needle exchanges shouldn’t just be used to manage a crisis — they should be put in place in time to prevent outbreaks from occurring. Clere has introduced a measure that would legalize needle exchanges across Indiana. When he introduced a similar measure last year, it failed and now, amidst the growing epidemic, Pence is still threatening to veto a needle exchange bill if it were to reach his desk.
Taking a page from New York’s experience when considering future steps
Every one of the infections in Scott County was utterly preventable — and each will cost, on average, $426,964, together totaling nearly $34 million, even if the epidemic is stopped immediately. Many of the people will now require HIV and HCV treatment at taxpayer expense. This could all be stopped with syringes that cost pennies. At the beginning of the 90s, New York’s injection drug users were facing an overwhelming epidemic. In 1990, before exchanges were fully legal here, 54% of New York’s roughly 200,000 injection drug users tested HIV positive. But by 2012, with needle exchange greatly expanded and prescription requirements for syringes dropped, that figure was down to a mere 3%. Though 30% to 50% of new infections were linked to IV drug use in the 1990s and 2000s, today that proportion is around 5%. And the number of new injectors has declined. A state report released last year, called needle exchange “the one intervention which could be described as the gold standard of HIV prevention.” New York’s decades of experience should be a lesson for Indiana, the federal government and the rest of the states that still limit needle access.
As stated in the CDC report, this “outbreak highlights the vulnerability of many rural, resource-poor populations to drug use, misuse, and addiction, in the context of a high prevalence of unaddressed comorbid conditions. The outbreak also demonstrates the importance of timely HIV and Hepatitis C surveillance activities and rapid response to interrupt disease transmission.” Syringe exchange programs need to be at the core of the treatment and prevention services. Stigma and politics need to be put aside to allow these programs to work as bridges to comprehensive treatment, prevention, and social services.
Latest
An International Human Rights Approach to Unregulated Pregnancy Centers
Sarah Wetter Rebecca Reingold Sophie Samson
The United Kingdom’s Decriminalization of Abortion: What the United States Can Learn from Abortion Criminalization in a Global Context
Rebecca Reingold Paulina Macías Ortega



