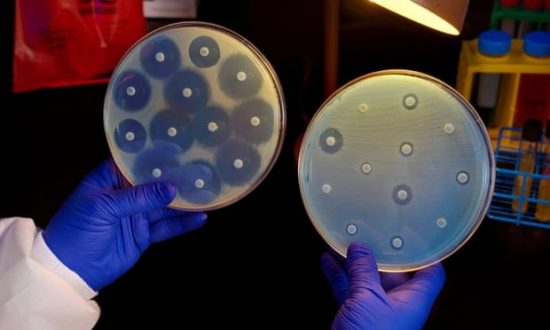
Will our future hold rapid growth in bacteria resistant to antibiotics (left) or susceptible to them (right)? That is still for policymakers and us to determine. Image courtesy of Science History Image/Alamy via The Guardian.
One of the greatest health threats of our time, one that grows by the year, is antimicrobial resistance. Bacteria and other microbes develop mutations that protect them against antibiotics and other antimicrobial drugs, meaning that infections, including deadly ones, that we can now treat will become more difficult — even possible — to treat. The 700,000 or more deaths that antimicrobial resistance now causes every year could grow to 10 million by 2050.
It could cause 10 million deaths per year by 2050. But just how likely is this?
Read an article or book discussing antimicrobial resistance, and you would think that without more action to combat resistance (such as by developing new antibiotics and other antimicrobials) and slow its spread (such as through more prudent use of existing antibiotics), we are on track to that truly frightening future. It would be a future where more people die of antimicrobial resistance than cancer, and today’s routine surgeries become dangerous – even too dangerous to undertake – because of the risk of deadly infections.
Bill Bryson’s general excellent book The Body: A Guide for Occupants (2019) puts it this way: “At the current rate of spread, antimicrobial resistance is forecast to lead to ten million preventable deaths a year” (p. 46). Bill Bryson cites a BBC Radio science program, whose host says that “the O’Neill report [to which we will return] suggests that [deaths from antibiotic resistance] will rise to 10 million people per year by 2050.” And he cites an article from Chemistry World, a news website developed by the United Kingdom’s Royal Society of Chemistry, which reports: “Already, drug-resistant bacterial infections kill 700,000 people every year…and authoritative sources suggest that this figure may rise to 10 million by 2050.”
Authoritative indeed. A New York Times article in December 2019 that warned of bankruptcies of antibiotic start-ups, threatening an already inadequate pipeline of new antibiotics, states, “Without new therapies, the United Nations says the global death toll could soar to 10 million by 2050.” And indeed, the United Nations said just that – though with emphasis on the word “could.” An April 2019 report from a UN interagency group stated: “Drug-resistant diseases already cause at least 700,000 deaths globally a year, including 230,000 deaths from multidrug-resistant tuberculosis, a figure that could increase to 10 million deaths globally per year by 2050 under the most alarming scenario if no action is taken” (p. 1). We will return to that key last phase of the UN statement about the most alarming scenario.
I could continue along these lines. Enter “10 million deaths antimicrobial resistance” into an Internet search engine, and you will find a plethora of examples like the news articles and programs cited above.
The origin of this 10 million figure – what we’re on track to reach “at the current rate of spread”, what “will” happen, what “may” or “could” happen – is a 2014 report by panel, the Review on Antimicrobial Resistance (AMR Review), that then-UK Prime Minister David Cameron had established earlier that year, chaired by Jim O’Neill. And it certainly gives that impression. A figure taking up an entire page (p. 5) of its December 2014 report (several more reports would follow) is labeled “Deaths attributable to AMR every year compared to other major causes of death,” with AMR in 2050 and its 10 million figure highlighted. And the report states, “Initial research, looking only at part of the impact of AMR, shows that a continued rise in resistance by 2050 would lead to 10 million people dying every year” (p. 6). Without looking more carefully, the way this figure has been reported in the press seems more or less accurate with respect to how the AMR Review characterizes its findings.
But keep reading, and the picture quickly becomes quite murky. The 10 million figure is drawn from two studies, which of which created possibly but hypothetical scenarios of what could happen in 2050.
One study, by the RAND Corporation, looked to three major infectious diseases and three bacteria where resistance is already a concern – AIDS, tuberculosis, and malaria, and Escherichia coli (E. coli), Klebsiella pneumoniae (K. pneumoniae), and Staphylococcus aureus (S. aureus) – and assumed in 15 years we would have no drugs to combat them. While resistance is a problem with all of these, there is no particular reason to believe that all drugs against them will cease to work, much less in fifteen years, which seems extremely unlikely – a “most alarming scenario” indeed, to use the UN interagency group’s words.
The other study, by KPMG, was similarly limited to the same six diseases and bacteria, and considered four different scenarios, varying by degree of resistance (40% or 100%) and rate of infection (as now, or all except for malaria doubling).
Among the two studies and multiple scenarios, the AMR Review fails to say exactly where its 10 million figure comes from. Review the two studies themselves, and you will not find that number.
One analysis in PLoS Medicine, referring to the 10 million figure, observes: “The scenario that seems to be underlying the most often quoted line entails a sharp initial rise of current resistance rates by 40 percentage points, after which rates remain stable until 2050, and doubled infection rates.”
This scenario, one of those from KPMG, does appear the most likely source to me as well; along with the RAND study, it is the scenario that the AMR Review itself highlights. Yet is that the most likely scenario? How much more likely is 10 million deaths than 5 million or 2 million – or are these or other lower tolls, in fact, actually (much?) more likely?
Notably, contrary to the scenario that seems to underlie the 10 million figure, presently HIV and TB infection rates are falling, not rising. While hardly representative of the world, but indicative of the possibilities of progress even at today’s level of insufficient action, the Center for Disease Control and Prevention’s best estimates (p. 16-17) indicate a slight decrease of annual antimicrobial resistance deaths in the United States, from 36,500 in 2012 to 35,900 in 2018.
What are we to make of all of this? First, what is, importantly, not the take-away.
That the 10 million death figure hardly reflects either current trends or is particularly more likely than millions fewer deaths (even as more deaths is conceivable as well) hardly means that antimicrobial resistance is not a major threat. It absolutely is, and with the problem worsening globally, a death toll that reaches into the millions annually is well within the realm of possibility.
Nor does the highly speculative models from the RAND Corporation and KPMG mean that we should generally distrust scientific models in general. Most notably, climate change models are based on vastly more data and evidence than these AMR models. They are not based on assumptions that could easily have been different, but on the collective knowledge of one of humanity’s greatest collaborative scientific undertakings ever, encompassing an immense number of studies and observations of both the past and present.
When we hear that there could be 10 million deaths in 2050 from antimicrobial resistance, we should take the general warning of the threat very seriously, but not the specific number. But when scientists tell us that we must take “rapid, far-reaching and unprecedented changes in all aspects of society” to avoid particularly disastrous levels of climate change, with a 45% reduction in greenhouse gas emissions (from 2010 levels) by 2030, we must achieve at least that level of reduction in that timeframe. This is even as 2030 is more of a critical benchmark than the singular turning point of humanity.
Nor should we distrust news outlets like the New York Times or the BBC. They did not intentionally mislead anyone. They just repeated the figures that the AMR Review presented, which had quickly become the go-to statistic, taking on a life of its own.
What we should take away are several lessons on how health (and other) information is should be presented. One, journalists should not add their own interpretation. For example, the AMR Review does not say that there will be 10 million deaths based on the current rate of spread – even though without a careful read, it is understandable that one might come away with this understanding.
Two, Carl Sagan famously said (drawing on similarly expressed sentiments of others), “Extraordinarily claims require extraordinary evidence.” That 10 million people will die from antimicrobial resistance annually (for reference, 56.7 million people died in 2015 [p. 10]) is an extraordinary claim. Journalists should take extra care in such cases to ensure that they are faithfully presenting the assertions. While the AMR Review does not explain where exactly the 10 million number comes from, it does suggest that it based on one of two scenarios (or some combination of both, the RAND scenario and the one that the PLoS Medicine analysis deemed most likely. Journalists should provide the full context so that their audience can understand just what the claim is. In this case, it is that under very specific assumptions – which the AMR Review does not clearly identify, nor justify as the ones it has chosen to highlight – there will be 10 million deaths annually by 2050.
Three, journalists should not strip critical context, like assumptions, when reporting predictions (or other information) using secondary sources. For example, given the highly respected sources Bill Bryson was referencing – the BBC and a publication of the Royal Society of Chemists – it is no wonder that he took the sources at face value, without seeking out the primary source. Yet neither of those sources provided any information about the assumptions underlying the 10 million estimate, or even that they are based on one specific scenario, not current trends or what is necessarily most probable.
And fourth and perhaps most significantly, those making extraordinary (or any) assertions should provide their reasoning. Yet as the PLoS Medicine article explained: “In the [AMR Review] chapter presenting the “10 million” estimate, exact numbers are reported without clear reference to background data, assumptions, or scenarios. Confidence intervals or results from sensitivity analyses are likewise omitted.”
In an era when high levels of distrust of scientific authorities has massive, lethal consequences – from lack of action to address the climate crisis to distrust in vaccines, leading to measles outbreaks – scientists and other health authorities, and journalists, must do all they can to rebuild that trust. Transparency is central. Blogs like this one should become a thing of the past.



